Breastfeeding and HIV/AIDS > Reducing Mother-to-Child Transmission of HIV among Women who Breastfeed
• Replacement Feeding: Transition to Replacement Feeding by HIV-Positive Women Who Breastfeed

 |
Spotlight on PMTCT:
Reducing Mother-to-Child Transmission of HIV among Women who Breastfeed
This publication is from LINKAGES Project.
Download pdf 4 Pages - 88 kb -  English, French - Alternate on-site download English, French - Alternate on-site download  English English
|
April 2004
A series of updates on critical infant and young child feeding issues
| The purpose of this issue of Spotlight is to provide decision makers, program managers, and health workers with guidance on how to support HIV-positive mothers who choose to breastfeed so that they can minimize the risk of transmission and protect their own health and the health of their infant. For many HIV-positive mothers in resource-limited settings, breastfeeding is the only or the safest infant feeding strategy available. |
The greatest threats to child survival in most communities are diarrhea and respiratory infections. Breastfeeding helps protect against these and other infections by providing antibodies and other protective factors, minimizing exposure to pathogens, and ensuring optimum nutrition. Interventions to protect and promote breastfeeding would prevent an estimated 13 percent of the 10 million deaths of children under five each year, making breastfeeding promotion one of the most effective child survival interventions available.1 In devising strategies to reduce mother-to-child transmission of HIV, these wider public health benefits of breastfeeding must be kept in mind.
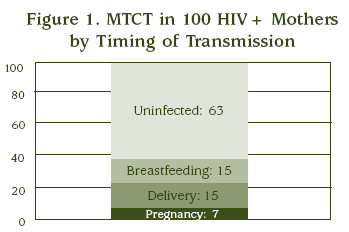
Most HIV-infected women do not transmit HIV to their infants. A mother can transmit HIV to her infant during pregnancy and delivery or through breastfeeding, but most babies of mothers with HIV are not infected. With no intervention to reduce transmission, 5–10 percent of infants will be infected during pregnancy, 10–20 percent during labor and delivery, and 10–20 percent through breastfeeding if breastfed for 18 to 24 months.2 Using the midpoints of these ranges, among 100 HIV-infected women, 7 of their infants will be infected with HIV during pregnancy, another 15 during labor and delivery; and another 15 over the course of about 2 years of breastfeeding. As shown in Figure 1, 63 infants will not become infected with HIV, even if breastfed and without any intervention in place to prevent transmission.
Promotion and support of optimal infant feeding practices should be part of all programs for the prevention of mother-to-child transmission (PMTCT) of HIV. Knowing the mother’s HIV status in pregnancy is the key to infant feeding counseling. Infant feeding decisions should be based on knowledge of the mother’s HIV status. Although most countries now offer voluntary and confidential HIV counseling and testing as part of antenatal services linked to PMTCT programs, actual uptake remains low. The challenge now is to improve these services and to expand coverage.
Even among mothers known to have HIV, the benefits of breastfeeding may outweigh the risks of transmission. An HIV-positive mother can avoid postnatal transmission by replacing breastmilk with commercial infant formula or home-modified animal milk from birth. However, in many resource -limited settings, these alternatives may be unavailable or too dangerous due to the risk of death from malnutrition, diarrhea, pneumonia, and other infections. When replacement feeding is not “acceptable, feasible, affordable, sustainable, and safe,” the United Nations agencies recommend exclusive breastfeeding “during the first months of life.” They recommend that “breastfeeding should be discontinued as soon as feasible, taking into account local circumstances, the individual woman’s situation, and the risks of replacement feeding.” 3
Risk Factors for Postnatal Transmission
Mother:
• Immune/health status
• Plasma viral load
• Breastmilk virus
• Breast inflammation (mastitis, abcess, nipple lesions)
• New HIV infection
• Viral characteristics |
Infant:
• Breastfeeding duration
• Non-exclusive breastfeeding
• Age (first months)
• Lesions in mouth, intestine
• Prematurity
• Infant immune response |
The risk of HIV transmission through breastfeeding can be reduced. The factors that contribute to postnatal transmission are listed in the box above. The HIV-infected mother who chooses to breastfeed can minimize these risks by guarding her own health, following feeding guidelines, and reassessing the risks as the infant ages and conditions change. The health provider, community worker, and program planner can support her and help in the following ways.
Infant Feeding Counseling
Counseling on safer breastfeeding practices should be a major component of efforts to reduce the risk of HIV transmission and increase child survival.
Provide adequate lactation counseling and support to prevent breast conditions. Improper positioning and attachment at the breast and infrequent feedings can cause cracked nipples and mastitis (an inflammation of the breast). A breast abscess—a localized collection of pus—usually results from untreated mastitis. Cracked nipples, mastitis, and breast abscess are three conditions associated with higher transmission of HIV through breastfeeding. Studies suggest that approximately 11–13 percent of HIV-infected women experience one or more of these conditions during breastfeeding, often during the early weeks when the risk of HIV transmission is thought to be greater. Preventable and treatable breast conditions may be responsible for up to half of HIV transmission through breastfeeding.4 Counseling on good breastfeeding techniques at the onset of lactation can help prevent breast problems. In a study in Bangladesh, the prevalence of severe inflammation of the breast was three times greater in women who had not received counseling than those who had.5
Counsel women to recognize breast conditions and seek treatment immediately. A breastfeeding mother with HIV should seek immediate treatment for cracked nipples, mastitis, and breast abscesses. If she has any of these conditions, she should express milk frequently from the infected or sore breast and discard it until the breast is healed.
Counsel on exclusive breastfeeding (feeding only breastmilk, with no other foods, fluids, or even water). For mothers who are HIV-negative or who do not know their status, exclusive breastfeeding is universally recommended as the optimal infant feeding practice for the first 6 months of life. Exclusive breastfeeding may also help reduce the risk of transmission among HIV-positive mothers who choose to breastfeed. Several studies are in progress to verify the results of a study6 in Durban, South Africa showing that infants partially breastfed before 3 months had higher rates of postnatal transmission compared with babies who had been exclusively breastfed for at least 3 months.
Assist families with decisions about transitioning from breastfeeding to replacement feeding (replacing breastmilk with a diet that provides all the nutrients the child needs). All infants of HIV-positive mothers will eventually reach an age when the balance of risks favors replacement feeding. Risks change over time. After the first few months of infancy, the risks associated with the use of breastmilk substitutes, such as infant formula and animal milk, are reduced, but the risk of HIV transmission through breastfeeding remains. Data suggest that breastfeeding after 6 months accounts for about 50 percent or more of all postnatal transmission. By 6 months the infant is better able to tolerate undiluted cow’s milk, goat’s milk, and a variety of semi-solid foods, so the options for replacement feeding become safer, less difficult, and less expensive than at an earlier age. For these reasons, some health experts recommend that mothers who choose to breastfeed should transition to replacement feeding at 6 months, a time when the introduction of soft and semi-solid foods should also take place.
The decision about when to stop breastfeeding should be based on an individual assessment of the health status of both the mother and the infant and the family’s ability to provide replacement foods. These foods should be appropriate for the infant’s age, safely prepared, and nutritionally adequate to ensure child growth and good health and development. Health providers and community workers can teach parents how to prepare replacement milks safely and help them address attitudes in the community toward women who do not breastfeed.
Antiretroviral Treatment and Prophylaxis
Antiretroviral treatment to keep HIV-infected mothers healthy may be one of the most important ways of preventing postnatal HIV transmission.
Treat the mother with a combination of antiretroviral (ARV) drugs. If available and clinically indicated,7 highly active antiretroviral therapy should be used to treat the mother to delay disease progression. In a study in West Africa,8 postnatal transmission (measured from 6 weeks through 24 months in breastfeeding infants) was 22 percent in mothers with baseline CD4* counts below 500/mm3 but only 2 percent among women with higher baseline CD4 counts. Both viral load and CD4 count are independently associated with the risk of transmission through breastfeeding. The World Health Organization recommends that if mothers taking ARV treatments to delay disease progression choose to breastfeed, they should continue their ARV regimen even though the effects on infant health and on transmission through breastfeeding have not yet been evaluated.9
Provide antiretroviral prophylaxis for PMTCT. In situations where combination therapy is either not indicated or not available, prophylactic therapy with antiretroviral drugs taken by the mother and infant about the time of delivery reduces the risk of perinatal transmission. Several regimens are approved for this purpose. The regimen most commonly used in resource-limited settings involves 200mg of nevirapine given orally to the mother at delivery and 2mg/kg given to the neonate within 72 hours. Trials are currently underway to evaluate the safety and efficacy of antiretroviral regimens taken by the mother and/or infant after delivery to prevent transmission through breastfeeding. Although preliminary results are encouraging, no regimens for postpartum antiretroviral prophylaxis have yet been approved.
Primary Prevention
Counseling on safer sex should be a component of PMTCT programs. The risk of transmission through breastfeeding is higher if the mother is newly infected during lactation.10
Promote safer sex to prevent infection of women who are not HIV infected. The higher risk of transmission through breastfeeding among newly infected mothers is thought to be due to the high level of virus in the mother after infection but before her immune system begins to fight the infection. Uninfected mothers can protect themselves and their breastfeeding infants from infection by practicing safe sex.
Supporting Nutritional Interventions
Nutritional interventions for the HIV-infected mother may improve her health and quality of life, provide additional nutrients to support pregnancy and lactation, and meet the increased energy needs resulting from the HIV infection.
Counsel the mother and her family on the importance of nutritional support and care. Nutritional care and support may be the only treatment to which the HIV positive mother has access. Reduced appetite, poor nutrient absorption, and physiological changes can lead to weight loss and malnutrition in HIV-infected people. Nutritional requirements are known to increase as a result of HIV infection and should be met by increased intakes of nutritious foods. Asymptomatic HIV infection increases energy needs by an estimated 10 percent, and symptomatic infections increase requirements by up to 30 percent.
Some micronutrient supplements have been shown to improve the survival of HIV-infected adults with more advanced infection. Although adequate micronutrient intake is best achieved through an adequate diet, multiple micronutrient supplements may be needed in pregnancy and lactation in some settings. Due to concerns about the possible negative effects of certain micronutrients in excess of requirements, WHO currently recommends that intake by HIV-infected women not exceed “recommended daily allowance” levels.
Lactation also increases nutritional requirements. To support lactation and maintain maternal reserves, breastfeeding mothers (whether infected or not) should consume the equivalent of about one extra meal (650 Kcal) per day. Normally, mothers are hungrier and thirstier during lactation and will satisfy this need if food and drink are available. HIV-infected mothers with reduced appetites can be encouraged to eat well by ensuring that food is available, appetizing, and nutritious.
Together the interventions outlined in this document can increase child survival and enable families to take positive actions to protect the health of both mother and child.
* CD4 cells are a component of the immune system attacked by HIV. Low CD4 counts are therefore both an indicator and a functional consequence of advanced HIV infection.
Acknowledgment: This issue of Spotlight draws upon a paper4 and presentations by Ellen Piwoz, SARA Project and Jay Ross, LINKAGES Project.
Endnotes
1 Jones G, Steketee RW, Black RE, Bhutta ZA, Morris SS and the Bellagio Child Survival Study Group. How many child deaths can we prevent this year? Lancet 2003;362:65-71.
2 De Cock KM, Fowler MG, Mercier E, de Vincenzi I, Saba J, Hoff E, Alnwick DJ, Rogers M, Shaffer N. Prevention of mother-to-child HIV transmission in resource-poor countries: translating research into policy and practice. JAMA 2000;283:1175-1182.
3 WHO. New data on the prevention of mother-to-child transmission of HIV and their policy implications. Conclusions and recommendations. WHO technical consultation on behalf of the UNFPA/UNICEF/WHO/ UNAIDS Inter-Agency Task Team on Mother-to-Child Transmission of HIV. Geneva, 11-13 October 2000. Geneva: World Health Organization, 2001, WHO/RHR/ 01.28.
4 Piwoz E, Ross J, Humphrey J. HIV transmission during breastfeeding: knowledge, gaps and challenges for the future. In: Advances in Experimental Medicine and Biology. Protecting infants through human milk: advancing the scientific evidence base. USA: Kluwer Publishing, (in press).
5 Flores M, Filteau S. Effect of lactation counselling on subclinical mastitis among Bangladeshi women. Ann Trop Paediatr 2002;22:85-88.
6 Coutsoudis A, Pillay K, Kuhn L, Spooner E, Tsai W-Y, Coovadia HM. Method of feeding and transmission of HIV-1 from mothers to children by 15 months of age: prospective cohort study from Durban, South Africa. AIDS 2001;15:379-387.
7 WHO. Scaling up antiretroviral therapy in resourcelimited settings – 2003 Revision (DRAFT). Geneva: World Health Organization, 2003.
8 Leroy V, Karon JM, Alioum A, Ekpini ER, Meda N, Greenberg AE, Msellati P, Hudgens M, Dabis F, Wiktor SZ. Twenty-four month efficacy of a maternal short course zidovudine regimen to prevent mother-to-child transmission of HIV-1 in West Africa: West Africa PMTCT Study Group AIDS 2002;16:631-641.
9 WHO. Antiretroviral drugs and the prevention of mother-to-child transmission of HIV infection in resource- constrained settings. Recommendations for use, 2004 Revision (DRAFT: 7 January 2004). Geneva: World Health Organization, 2004.
10 Dunn DT, Newell ML, Ades AE, Peckham C. Risk of human immunodeficiency virus type 1 transmission through breastfeeding. Lancet 1992;340:585-588.
Spotlight: PMTCT: Reducing Mother-to-Child Transmission of HIV among Women who Breastfeed is a publication by LINKAGES: Breastfeeding, LAM, Related Complementary Feeding, and Maternal Nutrition Program, and was made possible through support provided to the Academy for Educational Development (AED) by the Bureau for Global Health of the United States Agency for International Development (USAID), under the terms of Cooperative Agreement No. HRN-A-00- 97-00007-00. The opinions expressed herein are those of the author(s) and do not necessarily reflect the views of USAID or AED. April 2004
